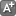Publisher's note: This post appears here courtesy of the Carolina Journal, and written by Julie Havlak.
Dr. Carrie Castille is examined by a new telemedicine device used to examine patients while instantly transmitting the physical assessment back to an off-site nurse practitioner. | Photo: Preston Keres/USDA
The coronavirus forced reforms that could help patients access telemedicine and affordable health care, experts said during the "COVID-19 and Telehealth: A New Era In Virtual Care"
Shaftesbury Society meeting Monday, May 18.
COVID-19 transformed virtual health care in North Carolina. The virus dismantled regulatory restrictions on telehealth, blocked in-person medical visits, and pushed providers to ramp up telemedicine programs across the state. But telemedicine still faces obstacles with privacy concerns, broadband access, and an uncertain regulatory future, says a
paper co-authored by John Locke Foundation and Brookings Institution researchers.
"An unlikely silver lining in all of this is that we have more telehealth," said
Jordan Roberts, John Locke Foundation health care policy analyst, at the virtual meeting.
"There are barriers that are hindering the adoption and use of telehealth right now. Simple regulatory changes can increase its use."
Before the pandemic, federal and state regulations choked telemedicine. Medicare covered telehealth only for seniors who lived in rural areas, and even they had to travel to designated medical facilities. Making matters worse, North Carolina banned physicians from treating patients across state lines. Private insurers mostly mimicked those restrictions.
Federal waivers let seniors access virtual care in the safety of their homes, and the CARES Act allowed providers to care virtually for new patients. The bill invested billions of dollars into telehealth programs and infrastructure. Some private insurers began temporarily covering telemedicine for the coronavirus.
"What COVID-19 did was unmask the emperor and take off all the clothes, because we had to get quality health care," said Nicol Turner Lee, Brookings Institution fellow.
"We have an opportunity to get more ubiquitous health care out there."
Telemedicine could help break down disparities in health care by freeing people from the constraints of their communities, said Lee.
"It increases the quality of care by decreasing the cost," Lee said.
"It's clearly a benefit for people to get access to quality health care. It doesn't matter where you live, as long as you have broadband and a smartphone."
Dr. Brian Forrest of Apex has used telehealth for years as a direct primary care physician with cash-based pricing. When he opted out of the insurance system, he escaped most regulatory restrictions on telemedicine.
Even before the outbreak, Forrest used telemedicine to treat his patients outside his office for their convenience. Now telemedicine has become critical to his practice's survival.
"It allowed me to extend my care beyond the four walls of the office," Forrest said.
"During COVID-19, this has really been a lifeline for our patients and our practice."
North Carolina temporarily mandated parity — requiring insurers to pay providers the same amount for in-person or virtual visits. The move aimed to shield providers financially during the outbreak.
"This is one of the biggest points of debate in the whole telehealth discussion," Roberts said.
"This can play out better with free negotiations between insurers and providers. ... To mandate that it must be paid at a certain rate seems counterintuitive to this cost-effective method."
Regulators should aim to create a broad, flexible framework that doesn't shut out new technologies, said Jack Karsten, Brookings Institution senior research analyst.
"Allow doctors to use innovative technology," Roberts said.
"Remove these barriers that have inhibited access to this great technology that can connect people over long distances. It's stopped at our state lines because of the way our regulations are written."
But providers worry telemedicine reforms won't outlast the crisis.
"COVID-19 has opened a lot of people's eyes to the possibilities of telemedicine, and we don't want to backslide," Forrest said.
"If policy makers let these loosened regulations roll back, if they don't go to interstate licensing, and allow some consistent level of reimbursement, you'll see a lot of physicians crawl back into their old comfort zone."